|
12/3/2023 0 Comments Protein turnover involves 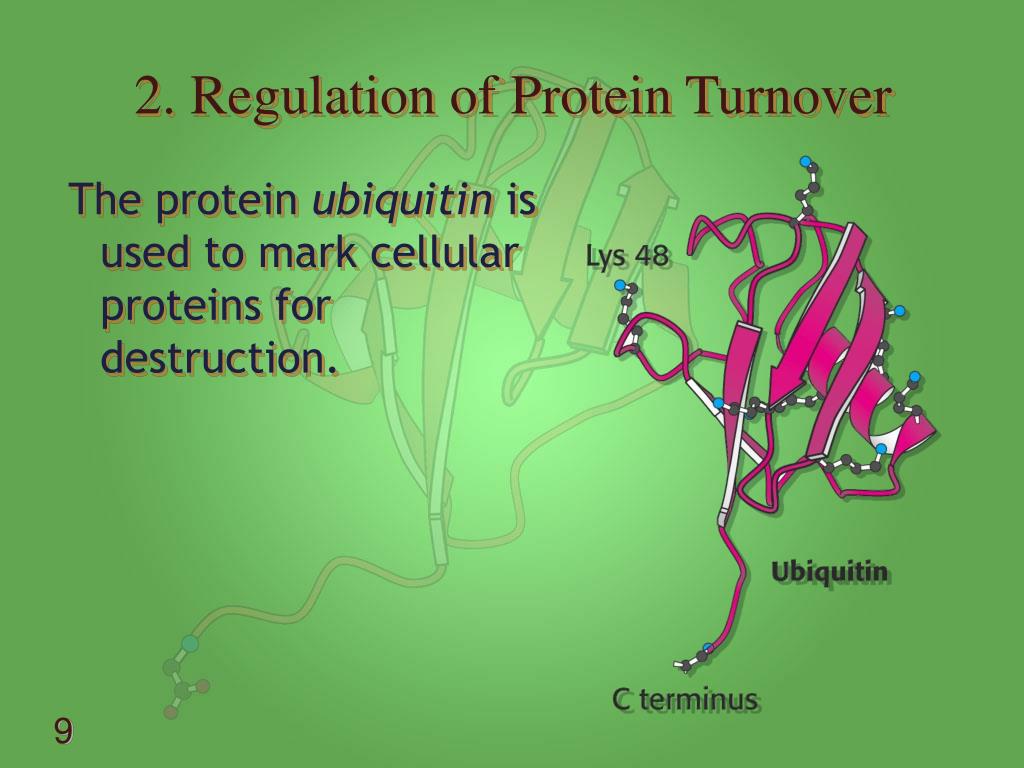 
The aim of this work is to review the mechanisms underlying the response of skeletal muscle to LPDs in CKD, while providing a summary of factors that increase the risk of protein wasting. In patients with CKD, an impaired ability to activate an adaptive response might impair N conservation when an LPD is prescribed. beyond the limits of the adaptive mechanisms. Of note, the concept of ‘adaptation’ to low-protein intakes has been separated from the concept of ‘accommodation’, the latter term implying a decrease in protein synthesis, with the development of wasting, when dietary protein intake becomes inadequate, i.e. Studies performed using stable isotope amino acid (AA) kinetics have shown that adaptation to dietary protein restriction involves a reduction in the rate of AA flux and oxidation, leading to more efficient use of dietary AA and a decrease in ureagenesis. Studies performed using the nitrogen (N) balance have shown that healthy young subjects can stay on neutral or even slightly positive balance with protein intakes as low as 0.55–0.6 g/kg. However, how and to what extent muscle protein metabolism adapts to decreased protein intake in humans is still largely unexplored. Skeletal muscle is a highly adaptive tissue that responds to hormones, substrate supply and exercise with changes in protein metabolism and ultimately in muscle composition and size. One major issue is our still incomplete understanding of the response of muscle metabolism to protein restriction in humans. Recent long-term randomized clinical trials on supplemented VLPDs in patients with CKD have shown a very good safety profile, suggesting that observations shown by short-term studies on muscle protein turnover can be extrapolated to the long-term period.ĬKD, low-protein diets, nutrition, protein BACKGROUNDĭespite the fact that protein restriction has been used for many decades in the treatment of patients with chronic kidney disease (CKD), there are still several unresolved issues regarding the metabolic effects of low-protein diets (LPDs). Current evidence shows that, in the short term, clinically stable patients with CKD Stages 3–5 can efficiently adapt their muscle protein turnover to an LPD containing 0.55–0.6 g protein/kg or a supplemented very-low-protein diet (VLPD) by decreasing muscle protein degradation and increasing the efficiency of muscle protein turnover. Acidosis, insulin resistance and inflammation are recognized mechanisms that can increase protein degradation and can impair the ability to activate an adaptive response when an LPD is prescribed in a chronic kidney disease (CKD) patient. Of note, the concept of ‘adaptation’ to low-protein intakes has been separated from the concept of ‘accommodation’, the latter term implying a decrease in protein synthesis, with development of wasting, when dietary protein intake becomes inadequate, i.e. Adaptation to a low-protein diet (LPD) involves a reduction in the rate of amino acid (AA) flux and oxidation, leading to more efficient use of dietary AA and reduced ureagenesis. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
